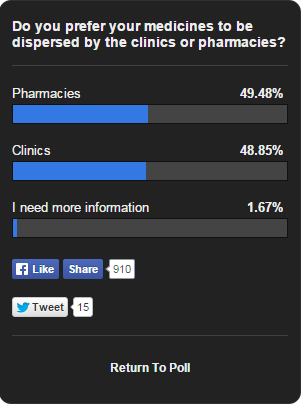
Is Malaysia ready for separation of dispensing? The patient perspective
Recently Astro Awani had a public opinion poll on this and the results are pretty evenly split (polls like this in any case can be manipulated by people who want to sway the votes and use nefarious tactics like bots and so on, so don’t take the results too seriously)
Both the pharmacy and doctors lobbies have been at it in the press and social media and presenting their side of the argument. You may also have seen this Astro Awani debate between a pharmacist and a doctor:
However at the end of the day, I think the perspective should be focused on the patient. Ultimately, will separation of dispensing benefit the patient?
Here are some salient points to consider from the patient’s point of view
1) Obtaining the medicines
There is no doubt that it is more convenient if the medicines are physician dispensed. While a pharmacist has argued that the exercise is good for you, patients who already feel sick may not be so inclined to have to travel to another location to get their medication. Availability of nearby pharmacies will be also limited particularly in the rural areas and by time of day since there are 24 hour clinics but no 24 hour pharmacies.
2) Choice of medicine
The doctors inventory is likely more limited than a well stocked pharmacy. There also may be cheaper generics available which the pharmacist can recommend which helps with the out-of-pocket paying patient. On the other hand, some doctors make the point that the medicines which they prescribe may not be available in the nearby pharmacies.
3) Safety
Medication errors always happen – humans will be humans. A pharmacist may for instance spot wrong dosages or medication interactions a doctor may have missed. However dispensing at the pharmacy is also not free of errors. Who is to check on the pharmacist? Dispensing errors may occur as a result of “bad doctors handwriting” (this can be overcome with a phone call to the doctor or by electronic prescription), but point-of-care dispensing will have less of this issue.
4) Information
Both doctors and pharmacists are supposed to explain to the patients details on their medication – what they are for, how to take them, possible side effects etc. A busy doctor may not have the time to provide a detailed explanation and this is where a pharmacist can compliment this aspect of patient education. On the other hand some explanation may require an intimate knowledge of the patient’s history and illnesses as well as an in-depth understanding of the disease, something the pharmacist may not have.
5) Cost
Will separation of dispensing increase or decrease the cost of healthcare? If the patient is paying out of his pocket, then it’s a big deal. The GP practice in Malaysia is quite unique. Many GPs do not charge much for consultation (in practice only a fraction of what they are allowed to under the PHFSA) being able to offset this with the sale of drugs at the clinics. If you separate dispensing, then the overall cost of healthcare will go up as GPs will have no choice but to increase their consultation charges. The argument for reduction of cost with separation of dispensing is that there will be a tendency to fewer unnecessary prescriptions.
A Taiwanese study showed that separation of dispensing did not help reduce total health expenditure.
6) Compliance
The rate of non-compliance is higher if there is separation of dispensing. Studies have shown that up to 30% of patients never get their prescriptions filled and physician dispensing results in better medication adherence rates. This is naturally an important point for the patient’s medical outcome. In the US, there is now a push for physician dispensing not only from a compliance perspective but also it may reduce billions in healthcare costs
So there you have it. We have tried to list out in a balanced fashion the arguments for and against separation of dispensing from the patient’s perspective – what is good and what is not good for the patient.
Is there a clear cut winner?
Tell us in your comments (Facebook login required as we only allow comments from those with Facebook accounts).